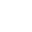What are Large Ankles?
Understanding and Addressing Large Ankles: Causes and Solutions

What Conditions Can Cause Enlarged Ankles?
Several factors can contribute to the development of large ankles:
1. Injury or trauma: Sprains, fractures, or other injuries to the ankle can lead to swelling.
2. Venous insufficiency: When the veins in the legs have difficulty returning blood to the heart, it can result in fluid accumulation and swelling in the ankles.
3. Lymphedema: This condition occurs when there is a blockage or damage to the lymphatic system, leading to fluid retention and swelling in various parts of the body, including the ankles.
4. Chronic conditions: Certain chronic health conditions like heart disease, kidney disease, liver disease, and arthritis can cause fluid retention and result in swollen ankles.
5. Pregnancy: Hormonal changes and increased pressure on the veins during pregnancy can lead to ankle swelling.
6. Medications: Some medications, such as certain blood pressure medications, hormones, or nonsteroidal anti-inflammatory drugs (NSAIDs), may cause fluid retention and result in swollen ankles.
Lipedema, What Causes Lipedema?
Lipedema is a chronic condition characterized by the abnormal accumulation of fat cells, primarily in the lower body, such as the hips, thighs, and legs. The exact cause of lipedema is not fully understood, but there are several factors that are believed to contribute to its development.
Hormonal factors: Lipedema predominantly affects women, suggesting a hormonal influence on the condition. It often begins or worsens during hormonal changes, such as puberty, pregnancy, or menopause. Hormones like estrogen are thought to play a role in the development of lipedema.
Genetic factors: There appears to be a genetic predisposition to lipedema, as it tends to run in families. Several genes have been identified as potential contributors to the condition, although more research is needed to fully understand the genetic basis of lipedema.
Lymphatic system dysfunction: Lipedema is commonly associated with impaired lymphatic system function. The lymphatic system plays a crucial role in fluid balance and immune function. When the lymphatic vessels are compromised, it can lead to fluid retention, inflammation, and the accumulation of fat cells characteristic of lipedema.
Inflammatory factors: Inflammation may also play a role in the development and progression of lipedema. Some studies suggest that chronic low-grade inflammation in the adipose tissue may contribute to the enlargement and proliferation of fat cells.
While these factors are believed to contribute to the development of lipedema, it's important to note that the condition is still not fully understood, and further research is needed to gain a complete understanding of its causes and underlying mechanisms.
Our mission is to create a world where every investment in modern beauty is Worth It.
Let's keep in touch
Get updates of the treatments you are interested
How is Lipedema Treated? How is Lymphedema Treated?
While there is no cure for lipedema, several treatment options can help manage the symptoms and improve quality of life for individuals with the condition. The primary goals of lipedema treatment include reducing pain, controlling swelling, improving mobility, and preventing further progression of the disease.
1. Conservative Measures:
Compression Therapy: Wearing compression garments, such as compression stockings or wraps, can help reduce swelling and provide support to the affected areas.
Manual Lymphatic Drainage (MLD): This specialized massage technique aims to improve lymphatic flow, reduce swelling, and enhance circulation.
Exercise: Engaging in low-impact exercises, such as swimming or walking, can help improve lymphatic flow, maintain muscle tone, and manage weight.
2. Surgical Interventions:
Liposuction: Lipedema fat is typically resistant to traditional weight loss methods. Liposuction techniques specifically designed for lipedema, such as tumescent liposuction or water-assisted liposuction (WAL), can help remove excess fat and reshape the affected areas. Liposuction can provide significant improvement in symptoms and body contour but is not considered a cure.
Lymphatic Liposuction: This is a specialized form of liposuction that aims to remove both excess fat and damaged lymphatic tissue to improve lymphatic flow and reduce swelling.
Combined Decongestive Therapy (CDT): It combines liposuction with manual lymphatic drainage and compression therapy to achieve better results in managing symptoms.
The best treatment approach may vary for each individual, and a personalized plan should be developed in consultation with a healthcare professional experienced in treating lipedema. Additionally, maintaining a healthy lifestyle with a balanced diet, regular exercise, and self-care practices can also be beneficial for managing symptoms and overall well-being.
How is Lymphedema Diagnosed?
Lymphedema is typically diagnosed through a combination of medical history evaluation, physical examination, and diagnostic tests. Here are the common steps involved in diagnosing lymphedema:
1. Medical history: The healthcare provider will discuss your symptoms, medical history, and any potential risk factors or events that may have contributed to the development of lymphedema. This can include surgeries, infections, radiation therapy, or a family history of the condition.
2. Physical examination: The healthcare provider will perform a thorough physical examination, paying close attention to the affected area. They will look for signs of swelling, skin changes (such as thickening or hardening), and any associated symptoms like pain or heaviness.
3. Measurement and comparison: The healthcare provider may use various tools to measure and compare the affected and unaffected limbs. This can involve measuring the circumference of the limbs at specific points and documenting any differences in size.
4. Lymphatic imaging: In some cases, imaging tests may be used to assess the lymphatic system and confirm the diagnosis. Imaging techniques like lymphoscintigraphy or lymphangiography can help visualize the flow of lymph fluid and identify any blockages or abnormalities.
5. Differential diagnosis: The healthcare provider will rule out other potential causes of swelling, such as venous insufficiency or deep vein thrombosis, to ensure an accurate diagnosis of lymphedema.
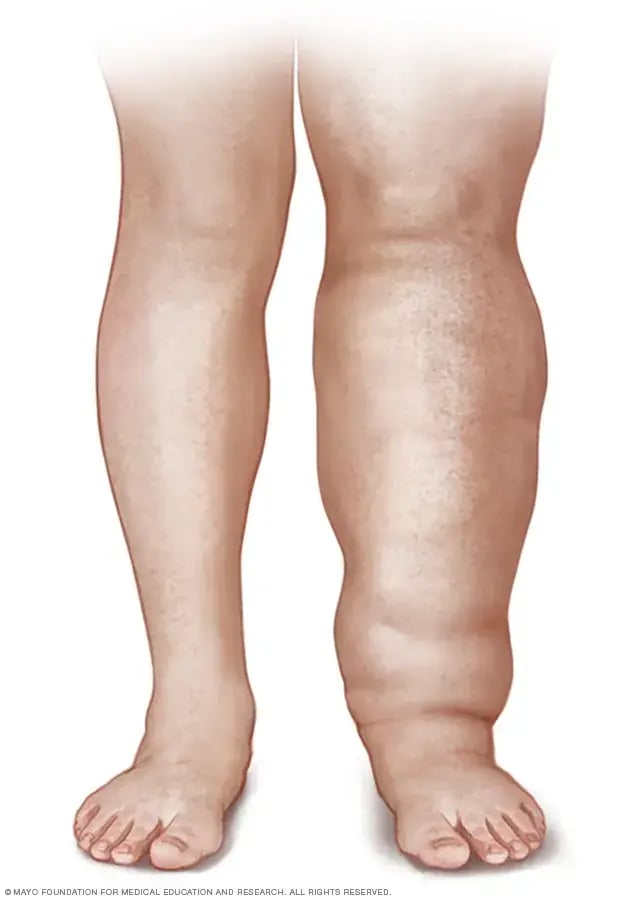
What You Can Do To Reduce the Size Of Your Ankles?
1. Elevate your legs: Elevating your legs above heart level can help reduce swelling in the ankles. Try to raise your legs on a pillow or cushion while lying down or prop them up on a footrest while sitting.
2. Compression stockings: Wearing compression stockings or socks can help improve circulation and reduce swelling in the ankles. These stockings apply gentle pressure to your legs, aiding in the movement of fluid back towards the heart.
3. Regular exercise: Engaging in low-impact exercises, such as walking or swimming, can promote circulation and reduce fluid retention. Exercise also helps to strengthen the muscles around your ankles, which can aid in reducing swelling.
4. Limit salt intake: Consuming excessive amounts of salt can contribute to fluid retention. Reduce your intake of processed foods, fast food, and adding extra salt to your meals. Opt for a diet rich in fruits, vegetables, lean proteins, and whole grains.
5. Stay hydrated: Drinking an adequate amount of water can actually help flush out excess fluid from your body. Although it may seem counterintuitive, dehydration can lead to water retention, so ensure you're staying hydrated throughout the day.
6. Medications: In some cases, medications may be prescribed to manage edema and reduce ankle size. Diuretics are commonly prescribed to increase urine output and remove excess fluid from the body. However, it's important to consult with a healthcare professional for proper diagnosis and to determine if medication is necessary for your specific situation.
Remember, these suggestions are not a substitute for professional medical advice. It's essential to consult with a healthcare provider to determine the underlying cause of your ankle swelling and develop an appropriate treatment plan.
Our mission is to create a world where every investment in modern beauty is Worth It.
Let's keep in touch
Get updates of the treatments you are interested
Understanding and Addressing Large Ankles: Causes and Solutions

What Conditions Can Cause Enlarged Ankles?
Several factors can contribute to the development of large ankles:
1. Injury or trauma: Sprains, fractures, or other injuries to the ankle can lead to swelling.
2. Venous insufficiency: When the veins in the legs have difficulty returning blood to the heart, it can result in fluid accumulation and swelling in the ankles.
3. Lymphedema: This condition occurs when there is a blockage or damage to the lymphatic system, leading to fluid retention and swelling in various parts of the body, including the ankles.
4. Chronic conditions: Certain chronic health conditions like heart disease, kidney disease, liver disease, and arthritis can cause fluid retention and result in swollen ankles.
5. Pregnancy: Hormonal changes and increased pressure on the veins during pregnancy can lead to ankle swelling.
6. Medications: Some medications, such as certain blood pressure medications, hormones, or nonsteroidal anti-inflammatory drugs (NSAIDs), may cause fluid retention and result in swollen ankles.
Lipedema, What Causes Lipedema?
Lipedema is a chronic condition characterized by the abnormal accumulation of fat cells, primarily in the lower body, such as the hips, thighs, and legs. The exact cause of lipedema is not fully understood, but there are several factors that are believed to contribute to its development.
Hormonal factors: Lipedema predominantly affects women, suggesting a hormonal influence on the condition. It often begins or worsens during hormonal changes, such as puberty, pregnancy, or menopause. Hormones like estrogen are thought to play a role in the development of lipedema.
Genetic factors: There appears to be a genetic predisposition to lipedema, as it tends to run in families. Several genes have been identified as potential contributors to the condition, although more research is needed to fully understand the genetic basis of lipedema.
Lymphatic system dysfunction: Lipedema is commonly associated with impaired lymphatic system function. The lymphatic system plays a crucial role in fluid balance and immune function. When the lymphatic vessels are compromised, it can lead to fluid retention, inflammation, and the accumulation of fat cells characteristic of lipedema.
Inflammatory factors: Inflammation may also play a role in the development and progression of lipedema. Some studies suggest that chronic low-grade inflammation in the adipose tissue may contribute to the enlargement and proliferation of fat cells.
While these factors are believed to contribute to the development of lipedema, it's important to note that the condition is still not fully understood, and further research is needed to gain a complete understanding of its causes and underlying mechanisms.
Our mission is to create a world where every investment in modern beauty is Worth It.
Let's keep in touch
Get updates of the treatments you are interested
How is Lipedema Treated? How is Lymphedema Treated?
While there is no cure for lipedema, several treatment options can help manage the symptoms and improve quality of life for individuals with the condition. The primary goals of lipedema treatment include reducing pain, controlling swelling, improving mobility, and preventing further progression of the disease.
1. Conservative Measures:
Compression Therapy: Wearing compression garments, such as compression stockings or wraps, can help reduce swelling and provide support to the affected areas.
Manual Lymphatic Drainage (MLD): This specialized massage technique aims to improve lymphatic flow, reduce swelling, and enhance circulation.
Exercise: Engaging in low-impact exercises, such as swimming or walking, can help improve lymphatic flow, maintain muscle tone, and manage weight.
2. Surgical Interventions:
Liposuction: Lipedema fat is typically resistant to traditional weight loss methods. Liposuction techniques specifically designed for lipedema, such as tumescent liposuction or water-assisted liposuction (WAL), can help remove excess fat and reshape the affected areas. Liposuction can provide significant improvement in symptoms and body contour but is not considered a cure.
Lymphatic Liposuction: This is a specialized form of liposuction that aims to remove both excess fat and damaged lymphatic tissue to improve lymphatic flow and reduce swelling.
Combined Decongestive Therapy (CDT): It combines liposuction with manual lymphatic drainage and compression therapy to achieve better results in managing symptoms.
The best treatment approach may vary for each individual, and a personalized plan should be developed in consultation with a healthcare professional experienced in treating lipedema. Additionally, maintaining a healthy lifestyle with a balanced diet, regular exercise, and self-care practices can also be beneficial for managing symptoms and overall well-being.
How is Lymphedema Diagnosed?
Lymphedema is typically diagnosed through a combination of medical history evaluation, physical examination, and diagnostic tests. Here are the common steps involved in diagnosing lymphedema:
1. Medical history: The healthcare provider will discuss your symptoms, medical history, and any potential risk factors or events that may have contributed to the development of lymphedema. This can include surgeries, infections, radiation therapy, or a family history of the condition.
2. Physical examination: The healthcare provider will perform a thorough physical examination, paying close attention to the affected area. They will look for signs of swelling, skin changes (such as thickening or hardening), and any associated symptoms like pain or heaviness.
3. Measurement and comparison: The healthcare provider may use various tools to measure and compare the affected and unaffected limbs. This can involve measuring the circumference of the limbs at specific points and documenting any differences in size.
4. Lymphatic imaging: In some cases, imaging tests may be used to assess the lymphatic system and confirm the diagnosis. Imaging techniques like lymphoscintigraphy or lymphangiography can help visualize the flow of lymph fluid and identify any blockages or abnormalities.
5. Differential diagnosis: The healthcare provider will rule out other potential causes of swelling, such as venous insufficiency or deep vein thrombosis, to ensure an accurate diagnosis of lymphedema.

What You Can Do To Reduce the Size Of Your Ankles?
1. Elevate your legs: Elevating your legs above heart level can help reduce swelling in the ankles. Try to raise your legs on a pillow or cushion while lying down or prop them up on a footrest while sitting.
2. Compression stockings: Wearing compression stockings or socks can help improve circulation and reduce swelling in the ankles. These stockings apply gentle pressure to your legs, aiding in the movement of fluid back towards the heart.
3. Regular exercise: Engaging in low-impact exercises, such as walking or swimming, can promote circulation and reduce fluid retention. Exercise also helps to strengthen the muscles around your ankles, which can aid in reducing swelling.
4. Limit salt intake: Consuming excessive amounts of salt can contribute to fluid retention. Reduce your intake of processed foods, fast food, and adding extra salt to your meals. Opt for a diet rich in fruits, vegetables, lean proteins, and whole grains.
5. Stay hydrated: Drinking an adequate amount of water can actually help flush out excess fluid from your body. Although it may seem counterintuitive, dehydration can lead to water retention, so ensure you're staying hydrated throughout the day.
6. Medications: In some cases, medications may be prescribed to manage edema and reduce ankle size. Diuretics are commonly prescribed to increase urine output and remove excess fluid from the body. However, it's important to consult with a healthcare professional for proper diagnosis and to determine if medication is necessary for your specific situation.
Remember, these suggestions are not a substitute for professional medical advice. It's essential to consult with a healthcare provider to determine the underlying cause of your ankle swelling and develop an appropriate treatment plan.